Abstract
INTRODUCTION: COVID-19 has disrupted healthcare access for patients (pts) with cancer, which may pose an especially high risk for pts with hematologic malignancies (NCI, 2021). The standard of care for newly diagnosed (ND) AML is induction with intensive chemotherapy (IC; "7+3") ± consolidation for eligible pts; while during the COVID era, lower-intensity regimens, such as a hypomethylating agent (HMA) plus venetoclax (VEN), may be recommended over 7+3 to eligible pts to minimize transfusions and inpatient hospitalizations. For pts who achieved remission from induction, COVID-19 may have led some practitioners to reduce the number of consolidation cycles and/or lower the cytarabine dose used for consolidation. Transplantation, including hematopoietic stem cell transplantation (HSCT), has been severely impacted (even halted in some areas) during COVID-19 (NasrAllah, 2021). The influence of COVID-19 on AML treatment (Tx) and outcomes has yet to be adequately studied.
OBJECTIVE: To assess the impact of COVID-19 on AML Tx patterns and survival in the real-world practice setting.
METHODS: The Flatiron™ EMR database was used in this retrospective analysis of US pts aged ≥ 18 years with an AML diagnosis between 1 Jan 2018 and 31 Jan 2021 and who had ≥ 2 months of follow-up. Tx patterns and survival outcomes were compared between a Pre-COVID cohort, defined as pts diagnosed with AML between 1 Jan 2018 and 31 Dec 2019, and a Post-COVID cohort of pts diagnosed between 1 Mar 2020 and 31 Jan 2021. Pt characteristics and Tx patterns were assessed for all pts and in the Pre- and Post-COVID cohorts using summary statistics. Time to event analyses used Kaplan-Meier methods for survival curves and were compared by log-rank tests.
RESULTS: In all, 2,133 pts met the selection criteria (mean age was 66.0 years, 57.5% were male, and 75.7% were treated in community practices); 1,582 (74.2%) pts were in the Pre-COVID cohort and 551 (25.8%) were in the Post-COVID cohort. Pt characteristics were generally similar between cohorts.
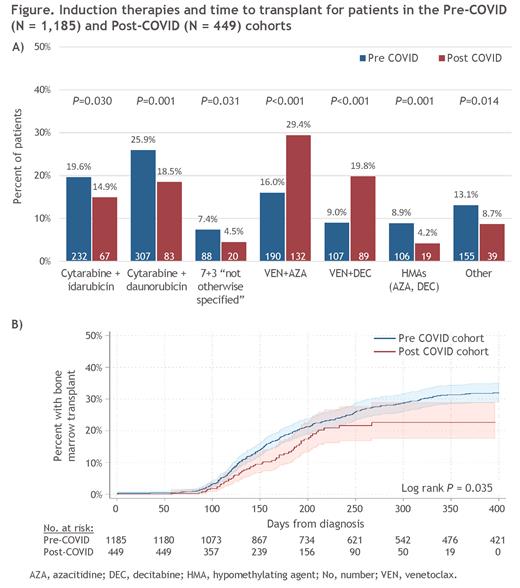
In the Post-COVID cohort, use of IC and HMA-only induction decreased significantly, while induction with VEN + an HMA increased (Fig. A): 29.4% of pts (n=132) in the Post-COVID cohort received VEN + azacitidine and 19.8% (n=89) received VEN + decitabine, compared with 16.0% (n=190) and 9.0% (n=107), respectively, in the Pre-Covid cohort (P < 0.001, both comparisons). Time to induction was shorter in the Post-COVID cohort vs the Pre-COVID cohort (median 14 vs 18 days; P < 0.001).
In all, 1,056 pts attained remission within 180 days of induction, including 774 Pre-COVID and 282 Post-COVID pts. Among them, 621 pts had a follow-up period of ≥ 180 days (394 pts Pre-COVID, 227 pts Post-COVID) and 41.1% (n=162) vs. 14.1% (n=32) of pts in the Pre- and Post-COVID cohorts, respectively, received consolidation (P < 0.001). Proportions of pts receiving maintenance therapy (MT) were 23.9% (n=94) and 17.6% (n=40) in the Pre- and Post-COVID cohorts, respectively (P = 0.069).
Time to HSCT was significantly increased for pts in the Post-COVID cohort (P = 0.035; Fig. B), and rate of HSCT was reduced for Post-COVID pts vs Pre-COVID pts (19.0% vs 13.3%, respectively, at 180 days, and 31.3% vs 22.7% at 360 days). Estimated overall survival (OS) was significantly longer in the Pre-COVID cohort (P = 0.006 vs. Post-COVID); at 360 days of follow-up, estimated survival rates in the Pre- and Post-COVID cohorts were 68.3% vs. 51.3%, respectively.
CONCLUSIONS: Induction with IC and HMAs was less frequent for pts diagnosed with AML during COVID-19, while induction with VEN + an HMA increased in these pts. Use of consolidation significantly decreased during COVID-19, and use of MT also decreased. These changes may have been influenced by inpatient resource constraints. Compared with the Pre-COVID cohort, Post-COVID pts were significantly less likely to receive HSCT, and longer HSCT waiting times suggest the pandemic affected access to timely transplantation, potentially due to hospital policies limiting surgeries, lack of available inpatient beds, or donor reluctance to visit a hospital during the pandemic. OS and 1-year survival were compromised in the Post-COVID cohort vs Pre-COVID pts, likely due to COVID-19 infection, but perhaps in part due to constraints on access to healthcare resources. These data suggest a need for oral Tx that can prolong remission while reducing clinic and inpatient visits, and that can bridge the gap until HSCT.
Chen: Bristol Myers Squibb: Current Employment, Current equity holder in publicly-traded company. Rotter: SmartAnalyst Inc.: Current Employment. Potluri: Bristol Myers Squibb: Consultancy.

This feature is available to Subscribers Only
Sign In or Create an Account Close Modal